
Sarasota Memorial's Nurse Residency Program Aims to Halt a Nursing Crisis
Editor's note: 2020 was designated the Year of the Nurse by the World Health Organization. And here, in the U.S., today is National Nurses Day. No one could have imagined how front and center nurses would become this year. What health care experts and hospital administrators have known is that the U.S. is facing a shortage of R.N.s; in Florida, that shortfall could happen as early as 2025. A local pilot project, the Suncoast Nursing Action Coalition (SNAC), is helping to train nurses in Sarasota, Manatee, DeSoto and Charlotte counties through an innovative mentoring program with Sarasota Memorial Hospital that pairs new nurses with experienced nurses during a 12-week program. Ironically, that mentorship program is on pause during the pandemic as hospitals were forced to furlough staff and implement hiring freezes, so SNAC’s program is on hold. “No one wants extra people in the hospital right now,” says Kate Graber, SNAC’s nurse navigator. In the meantime, SNAC is supporting and awarding scholarships to nurses who are getting their B.S.N. degrees and doctorates. Two years ago, we shadowed one of these nurses.
It’s 7:30 a.m. on a Wednesday in February, and the 10th floor of Sarasota Memorial Hospital’s Courtyard Tower buzzes with nurses changing shifts. Among them: Mariah Summerall, 27, who is taking notes on feeding needs, fall risks and what kind of attention patients will likely need over the next 12 hours. The floor is filled with patients with respiratory issues. Flu season is pushing the pace. Almost every bed is occupied.
Summerall, scribbling frantically on a sheet of paper, has been a full-time nurse for half an hour.
“It’s like the first day of school,” says Summerall, just one month after graduating from State College of Florida with her associate nursing degree. The first in her family to go to college, Summerall—who was born at Sarasota Memorial—paid her tuition by working as a patient care technician on this same SMH floor, spending the past two years here in a tech’s pale-blue uniform.
Now, a Hello Kitty pin, a college graduation gift from a friend, adorns her navy blue nurse’s scrubs just above a nametag that reads, “Mariah, R.N.” Her nerves haven’t overtaken her enthusiasm. “I got up this morning, I was like, ‘I’m ready to go to work!’” she says.
Summerall is part of a big push in American nursing to shrink the nationwide nursing shortage—a looming crisis—while improving skills.
The critical demand for hospital nurses is the result of an aging population combined with staggering workforce attrition. About 34 percent of newly licensed nurses who work in hospitals leave their jobs within two years. And a wave of retirements is coming. Of Florida’s current R.N.s, 44 percent are over the age of 50. The Suncoast Nursing Action Coalition (SNAC)—a pilot project in Sarasota, Manatee, DeSoto and Charlotte counties—reports that Florida may face an overall shortage of R.N.s as soon as 2025.
At the same time, Sarasota Memorial and hospitals across the country are pushing to make a B.S.N., a bachelor of science degree in nursing, the standard level of education since the degree is correlated with lower death rates, reduced disease and infection rates, and fewer complications. (Most nurses in the country have a two- to three-year associate of science nursing degree.) Currently, only a third of Southwest Florida nurses have a B.S.N. A national campaign led by the National Academy of Medicine is pushing for 80 percent of nurses to have their B.S.N. by 2020.
“There are millions of associate nurses producing excellent outcomes, but a B.S.N. education is more aimed toward critical thinking and leadership,” says Kate Garber, SNAC’s nurse navigator, who helps students and existing nurses get their B.S.N.
B.S.N. nurses are also one step closer to graduate nursing degrees, which qualifies them for the much-needed faculty positions responsible for producing subsequent crops of qualified nurses.
As a member of SMH’s 14-month nurse residency program, Summerall will spend the first 12 weeks of her career paired up with an experienced nurse preceptor, or coach, who will provide support. The terms of her hire also include a two-year obligation to SMH, during which Summerall is required to pursue her B.S.N. For that, SMH will reimburse her full tuition.
For today, Summerall and the 14 other beginning nurses in this residency class are stepping into their careers with a veteran nurse by their sides.
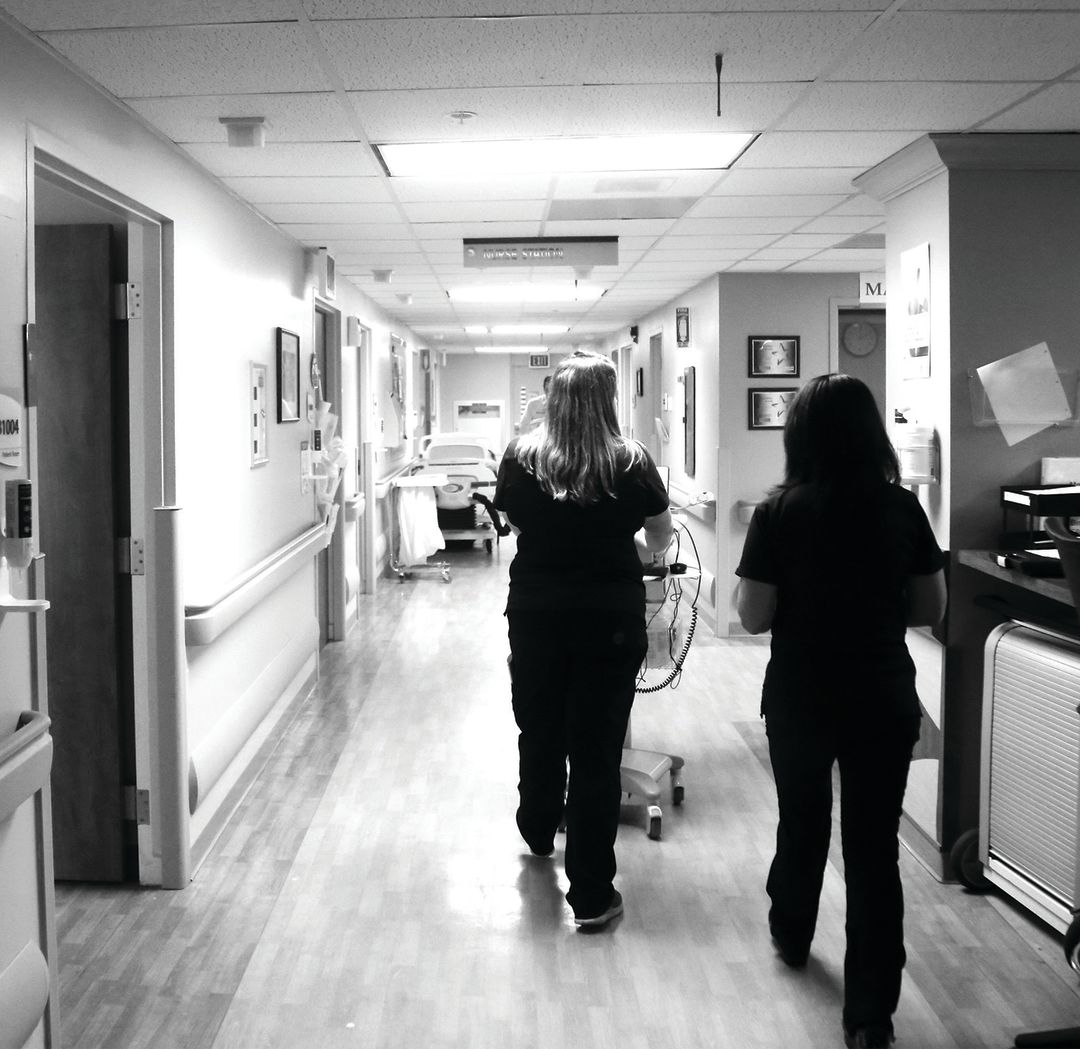
Image: Chad Spencer
For Summerall, that veteran nurse instructor is Kathleen Faticone, a dark-haired 50-something nurse with a charismatic, no-nonsense New York accent.
Summerall has been thinking about nursing as a career for a while. She was 10 when her grandmother was admitted to hospice. Then in her late teens, while an uncle underwent end-of-life care, Summerall befriended a hospice nurse who spoke with her about the challenges of caring for the terminally ill. Before Summerall had revealed her career plans, the nurse had already pegged her for a natural. “She told me, ‘You have to do this [career],’” Summerall remembers. “She said, ‘This is your calling.’”
Faticone, on the other hand, came to nursing later in life. “I was a pharmacist my first go-round,” she says. “Then I got married, raised my kids.” When her marriage ended, she pursued bedside nursing—much more hands-on than the pharmacy. She went through SMH’s residency program two years ago while the hospital paid for her B.S.N. degree. She’s an ardent supporter of her 10th-floor peers, both new and veteran.
“The culture of the unit is paramount,” she says. “I went through this program as a new nurse. They elevated me. We’re going to take that [new nurse] who’s really green, and we’re going to bring them up to our standards.”
And those standards are high. SMH is among only 6 percent of U.S. hospitals to earn a Magnet “Excellence in Nursing” award from the American Nurses Credentialing Center (ANCC). While most hospitals implement their own approach to new nurse orientation, SMH’s nurse residency program in 2017 became one of only two in Florida—and only 10 in the nation—to earn ANCC’s accreditation with distinction.
As Faticone and Summerall discuss the day ahead, a few instrumental bars from Brahms’ Cradle Song lullaby drift down from ubiquitous ceiling speakers, indicating a new admission to the mother/baby unit, four floors below.
Even in the best of circumstances, nursing is an act of priority juggling; a simple request, a new symptom or a sudden emergency code might be thrown in at any moment. Every additional patient represents that many more balls to keep in the air.
In some nursing homes or rehab facilities, a single R.N. can be responsible for dozens of patients at a time. A hospital floor nurse may have six or seven. SMH typically assigns its floor nurses to no more than five patients at a time; a two-nurse residency team like Faticone and Summerall starts out with a maximum of three patients.
During her clinical training, Summerall experienced patient-heavy environments at other facilities. “You’d leave feeling like there’s no way that you did everything to the best of your ability,” she says, “and that’s a crappy feeling.” That emotional toll can lead to a vicious cycle: When organizations suffer high nurse turnover, patient safety suffers. Nurses who do stay risk losing their licenses through stress-induced accidents or negligence.
Instead, just like the hospice nurses who inspired her, Summerall looks forward to building patient relationships while keeping an eye on their progress. “I like to see the difference you can make,” she says.
Faticone, says it takes emotional energy to build those relationships, over and over again.
“Every room you go in as a nurse, you’re going to talk differently,” she says. “Sometimes that’s hard to do. It’s hard to switch your psyche from one room to another.”
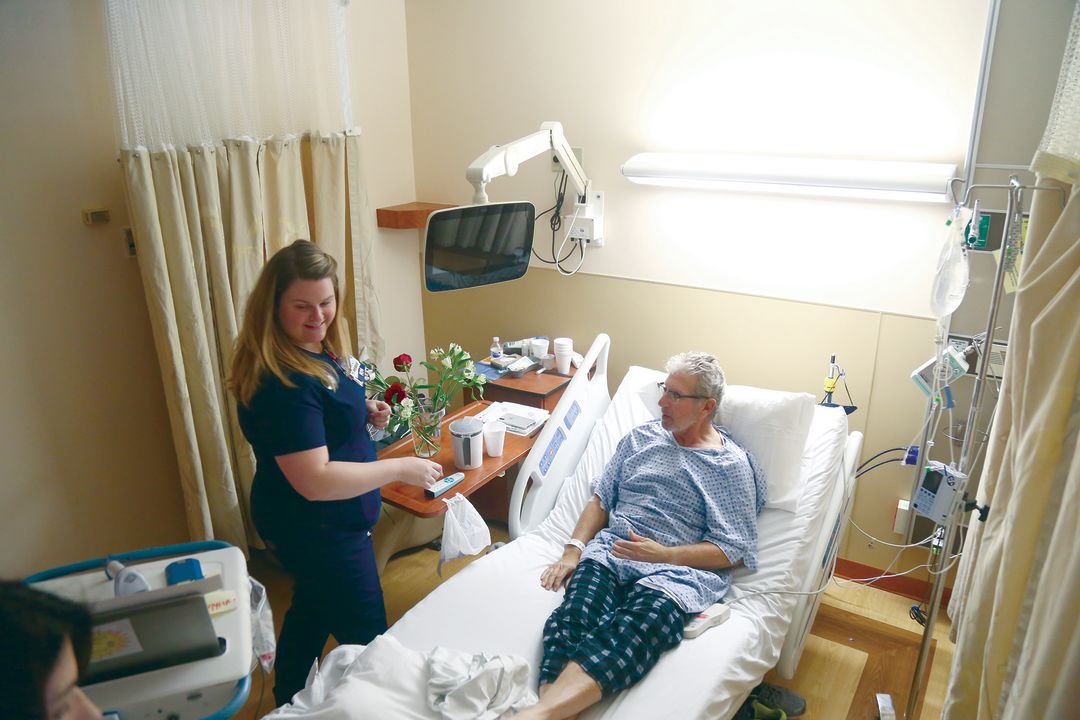
Faticone and Summerall discharging one of their patients, Mike Goldsmith.
Image: Chad Spencer
Around midday, Faticone and Summerall get the go-ahead to discharge one of their patients, Mike Goldsmith, a jovial, fit-looking, middle-aged man who jokes that his digestive issues were caused by “too much health food.” Faticone removes his IV and gives him his discharge instructions; Summerall passes him one last dose of potassium. Passing meds (making sure the patient and circumstance match the medication type and dosage) is one of the first, most vital skills nurses must master, along with patient assessment and documentation.
“The first week she’s doing those three things,” Faticone explains, “[while] I’m the one talking to the doctor, answering the phone calls, talking to family—basically picking up all the other nursing tasks. Because if you can’t get those first three down well, you cannot progress to the rest of it.”
Summerall says passing meds is the scariest part for her. “You’re the last person between the medicine and that person,” she says.
Faticone tells Summerall to avoid procrastinating—on anything. “If you have time, and it’s early in the day, you get ahead,” Faticone tells her. “You never say, ‘I’ll do it later.’ Because you’ll never catch up.”
As she says this, a man cries from a nearby room, “Hello? Hello?” Summerall grabs a pair of gloves from the wall dispenser and steps into the room, checking the whiteboard and addressing the patient behind a curtain. “Hey, Hank, what’s up? Yeah, you’re in the hospital, remember?”
This patient isn’t assigned to Summerall and Faticone, but Faticone says no one on the 10th floor walks past a blinking light or a cry for help. “They’re all our patients,” she says.

Summerall and Faticone listening to patient Marge Moran’s heart and lungs
Image: Chad Spencer
Before the end of their shift, Faticone and Summerall are assigned a new patient: Marge Moran, 82, admitted to the floor with low oxygen and trouble breathing. She’s a petite woman, with short, pale hair and a sweet smile.
The two nurses begin their assessment: “I’m Kathleen and that’s Mariah. You get two for the price of one today,” Fatticone says. “You’ve got a great view up here.” She points to a window overlooking midtown Sarasota and the bay. “This is the penthouse suite.”
Both nurses place their stethoscope diaphragms on Moran’s bare back. “Deep breath for me,” Faticone says to Moran. “I want you to smell the flowers and blow out the candles. Any pain? No pain anywhere? That’s what I like to hear.”
Moran whispers to Summerall that she’s hungry and can’t remember if she ate lunch. Summerall, who hasn’t eaten lunch herself, slips out of the room to retrieve a vanilla pudding for the patient as Faticone performs a final set of instructions. “I don’t think I have to tell you, but no smoking in the bathroom, no dancing in the halls,” she says with a wry smile. “Well, maybe a little dancing.”
Once Moran has finished her pudding, the two nurses will return to check her skin, all over. SMH’s patient population reflects Sarasota’s older demographics, and bed sores and falls remain constant concerns.
“Nursing is very intimate,” Faticone says later. “Can you imagine? We’ve just met, and I’m going to put my hands on her, and she’s naked. You have to build that trust very quickly.”
After two months on the job, Summerall has already matured. “You go into nursing and you’re like, ‘I’m going to save everyone,’” she says. “But you can’t always do that.”
Marge Moran never left the hospital. Six weeks after Summerall and Faticone admitted her, she died under the care of Sarasota Memorial’s in-house hospice. Summerall had visited her almost every shift, and she was one of the two nurses assigned to check the woman’s heart to certify the death. Moran’s daughters were present. “It was hard,” she says. “But I was OK.”
And since hospice is where Summerall wants to work, she feels reassured that she can handle the emotion of losing a patient with whom she’d forged a relationship and who used to say, “Hi, honey,” whenever she came by. “I like the dignity you can give people at the end of their lives,” she says.
Meanwhile, she’s gearing up to begin working on her B.S.N. while working full time. She’s also become more secure in passing meds, and in handling so many tasks and emotions at once. “I have a lot more confidence,” she says. “I do it over and over. There is a system. It’s overwhelming at first. I didn’t expect to feel so responsible for someone. You’re the one who notices the change in a patient. You’re the one who has to fight for your patient when they can’t stand up for themselves.”
Being a nurse, she says, “is everything I imagined and then some. I have a lot to learn, but I’m excited to go to work, and that’s a great feeling.”